Free Helpline
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
Chronic stress is now implicated in the pathology of heart disease, autoimmune conditions, digestive disorders, and cognitive decline. Understanding the biological mechanisms behind this damage is the first step in taking it seriously.
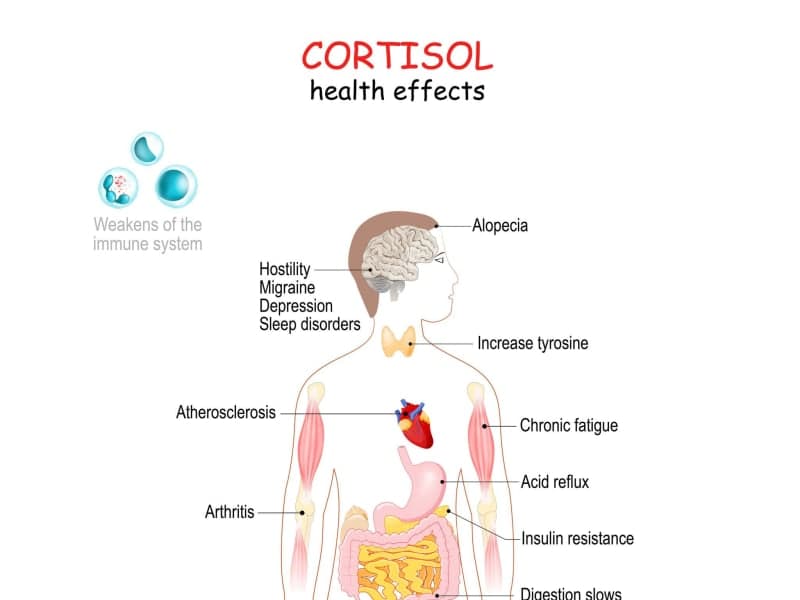
Chronic stress isn't just a mental health issue — it physically damages nearly every organ system. Here's what prolonged stress does to your body and how to interrupt it.
Stress is a normal physiological response to perceived threat — adaptive in acute situations, where cortisol and adrenaline mobilise energy, suppress non-urgent processes, and prime the body for action. The problem arises when this response becomes chronic: when the threat never resolves, the stress hormones never subside, and the body's normal recovery is perpetually deferred. Chronic stress physically damages nearly every major organ system in the body — not metaphorically, but through measurable biological pathways.
The hypothalamic-pituitary-adrenal (HPA) axis is the central stress response system. When the brain perceives a threat, the hypothalamus signals the pituitary gland, which signals the adrenal glands to release cortisol. In acute stress, cortisol spikes briefly and returns to baseline. In chronic stress, cortisol remains persistently elevated — or the HPA axis becomes dysregulated, producing erratic or blunted cortisol responses. This sustained disruption is the upstream cause of most physical damage associated with chronic stress.
Cardiovascular system: Chronic cortisol elevation raises blood pressure, promotes arterial inflammation, increases LDL oxidation, and elevates fibrinogen (a clotting factor). Research published in JAMA found that work-related chronic stress increases coronary heart disease risk by 40–50%.
Immune system: Short-term stress temporarily boosts immunity; chronic stress produces immune suppression, reducing natural killer cell activity and impairing vaccine response. Simultaneously, it elevates pro-inflammatory cytokines (IL-6, TNF-alpha), driving systemic chronic inflammation implicated in autoimmune disease, atherosclerosis, and cancer.
Brain and cognition: Prolonged cortisol exposure damages the hippocampus — a brain region essential for memory consolidation — reducing its volume over time. This is associated with impaired memory, executive function, and increased risk of depression and dementia. The prefrontal cortex, governing rational decision-making and impulse control, also atrophies under chronic stress exposure.
Gut and digestion: The gut-brain axis is bidirectionally disrupted by chronic stress. Cortisol increases intestinal permeability ("leaky gut"), alters microbiome composition, accelerates or slows gut motility, and exacerbates IBS, inflammatory bowel disease, and gastric ulcer formation.
Endocrine and reproductive systems: Chronic cortisol suppresses thyroid function, reduces testosterone and oestrogen, disrupts insulin sensitivity, and impairs sleep via melatonin interference — creating cascading hormonal dysfunction.
Telomere attrition: Research by Nobel laureate Elizabeth Blackburn found that chronic psychological stress is one of the strongest predictors of telomere shortening — a cellular marker of accelerated ageing.
Physiological sigh (double inhale through nose + long exhale): Shown by Stanford research to rapidly reduce physiological stress arousal in under 5 minutes
Regular aerobic exercise: Reduces HPA axis reactivity and normalises cortisol rhythm
Sleep prioritisation: Cortisol dysregulation and sleep deprivation create a vicious cycle; disrupting it requires both
Social support: Among the most powerful HPA axis buffers identified in human research
Chronic stress is a genuine physical health risk — not a personality trait or a sign of weakness. Its damage accumulates silently across years until it manifests as cardiovascular disease, immune dysfunction, cognitive decline, or metabolic disruption. Treating chronic stress with the same urgency as any other risk factor is not overreaction — it's evidence-based self-care.
1. What does chronic stress do to the body?
It damages the heart, brain, immune system, and hormones over time.
2. Why is chronic stress harmful?
Because prolonged cortisol disrupts normal body functions and recovery.
3. How can you reduce chronic stress?
Through exercise, good sleep, breathing techniques, and social support.
Author: Doctar Team
Disclaimer: For more information contact Doctar team.

Discover how eating impacts your blood pressure, learn about postprandial hypotension, and get practical diet tips for managing blood pressure, especially for Indian readers. Includes DASH and Mediterranean diet guidance.
April 1, 2026

Explore natural ways to support blood pressure management, including foods and herbs that may act like 'natural beta-blockers'. Learn about antioxidants, L-arginine, potassium, garlic, hawthorn, red yeast rice, and omega-3s. Always consult your doctor before making changes.
April 1, 2026