Free Helpline
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
Understand how Medicare covers physical therapy, including what's medically necessary, coverage limits, and different Medicare parts that may apply. Get practical tips for managing your PT costs.

Navigating healthcare coverage can feel complex, especially when you need physical therapy (PT). Many Indians undergoing rehabilitation or managing chronic conditions wonder about the costs involved and whether their insurance will help. This guide specifically addresses how Medicare, a significant health insurance program, covers physical therapy, offering clarity and practical advice for those who rely on it for their recovery and well-being.
If you're a Medicare beneficiary in India seeking physical therapy, understanding your coverage is key to managing your healthcare journey effectively. Medicare Part B is your primary resource for outpatient physical therapy that is deemed medically necessary. This means the therapy must be essential for diagnosing or treating a specific health condition or illness, or for slowing the worsening of your condition. It's not for general fitness or wellness.
For PT to be covered, it must involve skilled services provided by qualified professionals. This includes licensed physical therapists or doctors. Simple exercises for general fitness, for example, wouldn't qualify for Medicare coverage as physical therapy. Your therapist should always provide you with a written notice before offering any services that may not be covered by Medicare, allowing you to make an informed decision.
Once you have met your Medicare Part B deductible, which stands at $257 for 2025, Medicare will cover 80% of your physical therapy costs. This means you will be responsible for the remaining 20% as your out-of-pocket expense. A significant update is that there is no longer a cap on the total physical therapy costs that Medicare will cover, providing greater peace of mind.
Scenario: Imagine Mrs. Sharma, a 70-year-old woman recovering from a hip replacement. Her doctor prescribes intensive physical therapy three times a week. After meeting her deductible, Medicare Part B covers 80% of her sessions. While she pays the remaining 20%, the unlimited coverage means she can continue her therapy for as long as needed to regain full mobility without worrying about hitting a coverage limit.
There's a specific threshold after which your physical therapist must confirm that the services provided continue to be medically necessary for your condition. For 2025, this threshold is $2,410 in total PT costs. Beyond this point, your therapist needs to document the ongoing need for your therapy.
Furthermore, until 2028, if your total PT costs exceed $3,000, your claims might undergo a targeted medical review. It's important to know that not all claims are automatically subjected to this review process, but it's a possibility to be aware of.
Medicare Part A primarily covers inpatient hospital stays. This includes admissions to hospitals, mental health facilities, rehabilitation centers, and skilled nursing facilities. If you are hospitalized and require PT to improve your condition after your stay, Part A can cover these inpatient rehabilitation and PT services, provided they are medically necessary.
This is the most relevant part for most individuals seeking outpatient physical therapy. Part B covers medically necessary outpatient services, including PT aimed at diagnosing, treating, or improving your ability to function. You can receive this care in various settings:
Often called Medicare Advantage, these plans are offered by private companies approved by Medicare. They must provide at least the same coverage as Original Medicare (Parts A and B). Many Part C plans also offer additional benefits, such as coverage for dental, vision, and prescription drugs. If you have a Medicare Advantage plan, it will cover medically necessary physical therapy, often with similar rules to Part B, but check your specific plan details for any variations.
Medigap policies, also known as Medicare Supplement Insurance, can help cover out-of-pocket costs associated with Original Medicare. This includes deductibles, copayments, and coinsurance. If you have Original Medicare and pay a 20% coinsurance for physical therapy, a Medigap plan can significantly reduce your personal financial burden.
The cornerstone of Medicare coverage for PT is
Most people do not notice early warning signs right away. That is common. A simple symptom diary, basic routine checks, and timely follow-up visits can prevent small problems from becoming serious.
If you are already on treatment, stay consistent with medicines and lifestyle advice. If your symptoms change, do not guess. Check with a qualified doctor and update your plan early.
Write down symptoms, triggers, and timing for a few days.
Carry old prescriptions and test reports to your consultation.
Ask clearly about side effects, red-flag signs, and follow-up dates.
Seek urgent care for severe pain, breathing trouble, bleeding, fainting, or sudden worsening.
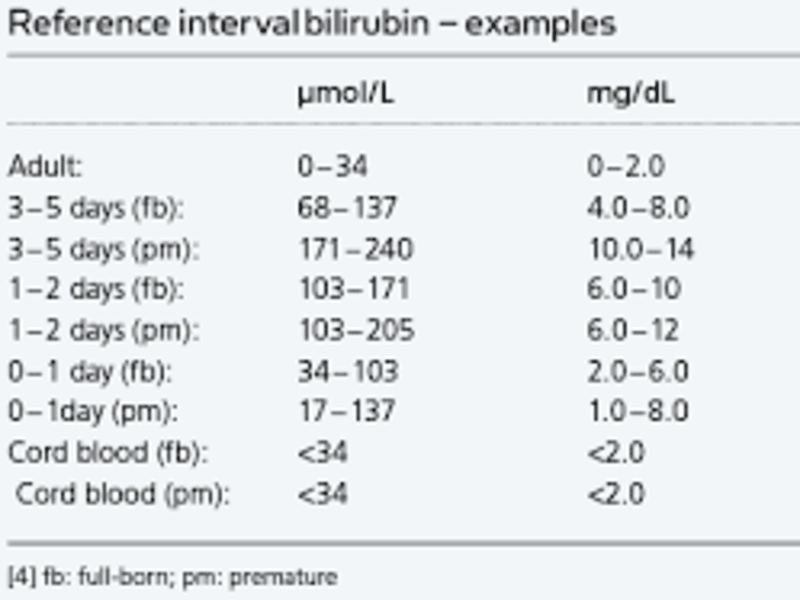
Bilirubin levels help assess liver health. This guide explains normal bilirubin values, types, causes of abnormal levels, symptoms, and when to seek medical advice.
April 11, 2026

Learn how to properly clean and care for your new ear piercing to ensure it heals beautifully and avoid infection. Follow our step-by-step guide for optimal results.
April 1, 2026

Discover practical, science-backed tips to sharpen your reaction time for gaming, sports, and everyday life. Learn how to improve your brain's speed and accuracy.
April 1, 2026