Free Helpline
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
Understand how Medicare covers echocardiograms (ECGs). Learn about costs, coverage under Parts A, B, and C, and what to do if your test isn't covered.

An echocardiogram, often called an echo or ECG, is a vital diagnostic tool that uses sound waves to create detailed images of your heart. It helps doctors assess your heart's structure, function, and blood flow, aiding in the diagnosis of various heart conditions. If you're a Medicare beneficiary in India, you might wonder if this essential test is covered by your plan. This guide aims to demystify Medicare coverage for echocardiograms, explaining what you can expect regarding costs and how different parts of Medicare apply.
An echocardiogram is a non-invasive imaging test that uses high-frequency sound waves (ultrasound) to produce pictures of your heart. It allows healthcare professionals to visualize:
Doctors order an echocardiogram to diagnose and monitor a wide range of heart conditions, including:
The straightforward answer is yes, Medicare generally covers echocardiograms when they are deemed medically necessary. This means your doctor must have a valid clinical reason to order the test based on your symptoms or existing health conditions. Medicare's goal is to ensure beneficiaries receive necessary medical care, and an echocardiogram often falls into this category.
However, your exact coverage and out-of-pocket costs can vary depending on which part of Medicare provides your coverage and where you receive the test.
Medicare Part A is your hospital insurance. If you are admitted to a hospital as an inpatient and your doctor orders an echocardiogram during your stay, Part A will typically cover it. The costs associated with the echocardiogram will count towards your Part A deductible. In 2025, the Part A deductible is $1,676 per benefit period. Once you satisfy this deductible, Part A covers all medically necessary tests and procedures, including echocardiograms, for the first 60 days of your hospital stay. This means if you're hospitalized for a serious heart event and need an echo, Part A steps in to cover the bulk of the cost after your deductible is met.
Medicare Part B covers outpatient medical services. If you need an echocardiogram as an outpatient – meaning you visit a clinic, doctor's office, or outpatient hospital department for the test without being formally admitted – Part B coverage applies. You'll need to meet your Part B annual deductible first. For 2025, this deductible is $257. After you meet the deductible, Medicare Part B will pay 80% of the approved cost for the echocardiogram. You will be responsible for the remaining 20% as coinsurance, plus any amount that exceeds Medicare's approved charge.
Scenario: Imagine you experience chest pain and your doctor's office schedules you for an outpatient echocardiogram. You've already met your Part B deductible for the year. Medicare will cover 80% of the test's approved cost, and you'll pay the remaining 20%.
Medicare Advantage plans are offered by private insurance companies approved by Medicare. These plans must provide at least the same coverage as Original Medicare (Parts A and B), but they often come with additional benefits and different rules. If you have a Part C plan, it will cover medically necessary echocardiograms. However, there are a few key points to remember:
Always check your specific Part C plan documents or contact your insurance provider to understand your coverage details, including network requirements and potential prior authorization needs.
The cost of an echocardiogram can vary widely, with median prices ranging from approximately $204 to $2,588. As a Medicare beneficiary, you typically pay less than those with commercial insurance or no insurance. Your out-of-pocket expenses will depend on:
If you have Original Medicare (Parts A and B), you might consider a Medigap policy. Medigap plans are sold by private insurance companies and can help cover some of the out-of-pocket costs that Original Medicare doesn't pay for, such as deductibles, copayments, and coinsurance for services like an echocardiogram. While Medigap policies have their own monthly premiums, they can provide significant financial relief when you need medical services.
Prior authorization is a process where your healthcare provider may need to get approval from Medicare or your Medicare Advantage plan before providing a service. For echocardiograms covered under Original Medicare (Parts A and B), prior authorization is typically not required. However, as mentioned earlier, some Medicare Advantage (Part C) plans might require it. This is determined by the specific insurance company that offers your Part C plan. It's essential to confirm with your provider and your plan administrator if prior authorization is a requirement for your echocardiogram.
To maximize your Medicare coverage for an echocardiogram, follow these steps:
If you believe Medicare should have covered your echocardiogram but didn't, you have the right to appeal the decision. Your Medicare Summary Notice (MSN) or Explanation of Benefits (EOB) will provide information on how to file an appeal. Gather all relevant medical documentation and follow the outlined appeal process. It's advisable to consult with your healthcare provider or a Medicare beneficiary support program for assistance with the appeal.
Medicare covers an echocardiogram whenever it is deemed medically necessary by your doctor. There isn't a strict limit on frequency as long as medical necessity can be established for each test.
The cost varies significantly. For Part B, after meeting the $257 deductible, Medicare pays 80% of the approved cost. Your share could be around 20% plus any costs exceeding Medicare's approved amount. For Part A during inpatient stays, costs are covered after the $1,676 deductible for the benefit period. Part C costs depend on your specific plan.
Generally, for an echocardiogram to be covered by Medicare, it must be ordered by a doctor. While not always a formal 'referral' in the sense of a separate document, your doctor's order documenting medical necessity is essential for coverage.
For Medicare to cover the test, you should get it at a facility that accepts Medicare. If you have a Medicare Advantage plan, you should prioritize facilities within your plan's network to ensure optimal coverage.
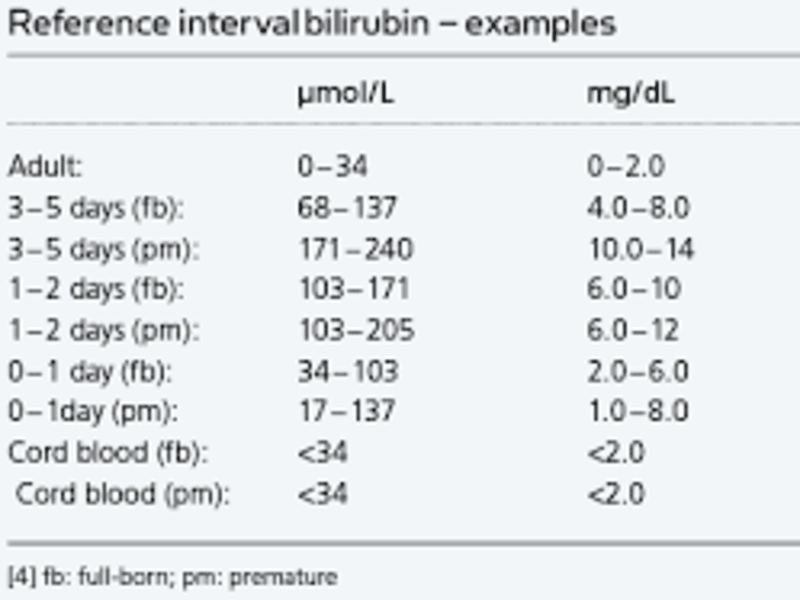
Bilirubin levels help assess liver health. This guide explains normal bilirubin values, types, causes of abnormal levels, symptoms, and when to seek medical advice.
April 11, 2026

Learn how to properly clean and care for your new ear piercing to ensure it heals beautifully and avoid infection. Follow our step-by-step guide for optimal results.
April 1, 2026

Discover practical, science-backed tips to sharpen your reaction time for gaming, sports, and everyday life. Learn how to improve your brain's speed and accuracy.
April 1, 2026