Free Helpline
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
Explore safe intimacy options beyond condoms, including internal condoms, diaphragms, and hormonal methods for pregnancy prevention. Understand their effectiveness and when condoms remain essential for STI protection.

When it comes to sexual health, using condoms is often the first line of defense recommended for preventing both sexually transmitted infections (STIs) and unintended pregnancies. They are highly effective when used correctly during penile-vaginal, penile-anal, and even penile-oral sex. However, for various reasons, some individuals may find condoms uncomfortable, experience allergies, or simply wish to explore other methods of protection. It's essential to understand that while condoms offer a unique dual benefit of STI and pregnancy prevention for penile sex, alternatives exist for specific situations, particularly concerning oral sex and internal barrier methods for those with vulvas.
Let's be clear: for penile sex, condoms remain the only method that offers significant protection against STIs and pregnancy simultaneously. They act as a physical barrier, catching ejaculate and reducing the risk of transmitting infections through bodily fluids. While no method is 100% foolproof, correct and consistent condom use dramatically lowers your risk. For those who find condoms a barrier to pleasure, exploring different types like ultra-thin or textured condoms can often enhance the experience. Brands like Trojan, Lola, and Skyn offer a variety of options to suit individual preferences. For individuals experiencing premature ejaculation, desensitizing condoms or thicker options from brands like Durex, Lifestyle, or Trustex can be beneficial.
When we talk about alternatives, it's important to distinguish between preventing pregnancy and preventing STIs. For oral sex, the protection against STIs is less about a barrier method and more about hygiene and awareness. However, for individuals with vulvas seeking pregnancy prevention or an additional layer of protection during specific acts, several options are available. It's crucial to remember that for penile sex, these alternatives do not offer the same level of STI protection as condoms.
The internal condom, sometimes referred to as a female condom, is a pouch that lines the vaginal or anal cavity. The FC2 internal condom, for example, is an FDA-approved, latex- and hormone-free option. While slightly more expensive than external condoms, it provides a good level of protection against pregnancy. It can be inserted up to 24 hours before intercourse, offering flexibility. However, its efficacy for preventing pregnancy is around 79% when used consistently and correctly.
A diaphragm is a dome-shaped device made of silicone that is inserted into the vagina to cover the cervix. It's typically used with spermicide to physically block sperm from reaching the egg. A diaphragm can be inserted up to 24 hours before intercourse and can remain in place for up to 48 hours, allowing for multiple sexual encounters within that timeframe. When used correctly with spermicide, diaphragms can be up to 96% effective in preventing pregnancy. However, their typical use effectiveness is lower, ranging from 77% to 83%, highlighting the importance of proper insertion and consistent use.
The contraceptive sponge is a soft, disposable foam device containing spermicide. It is inserted into the vagina to cover the cervix, aiming to block and kill sperm. While simple to use, the sponge is a single-use method and its effectiveness in preventing pregnancy is around 76% for those who have not given birth and slightly lower for those who have.
The withdrawal method, or the pull-out method, involves a partner withdrawing their penis from the vagina before ejaculation. This method relies heavily on timing and control. While it can prevent pregnancy if performed perfectly, its typical use effectiveness is only about 78%. This means that a significant number of unintended pregnancies occur when this method is used, and it offers no protection against STIs.
For pregnancy prevention, hormonal methods are highly effective. Oral contraceptive pills, commonly known as birth control pills, are one of the most popular reversible methods. They contain hormones (estrogen and progestin, or progestin-only) that prevent ovulation. When taken correctly, they are 98% to 99.7% effective. It's essential to consult with a healthcare provider to determine the best type of pill for your individual needs. The contraceptive patch is another option. This small patch is worn on the skin and releases hormones to prevent pregnancy. It's typically worn for three weeks with a one-week break. When used correctly, the patch can be up to 99% effective.
It's vital to reiterate that condoms are the only method that provides robust protection against STIs during penile sex. If you or your partner has multiple sexual partners, or if you are not in a long-term, mutually monogamous relationship where both partners have been tested for STIs, condoms are your most reliable safeguard. Even if you use other birth control methods for pregnancy prevention, consider using condoms alongside them to reduce STI risk.
Priya and Rohan are in a new relationship and want to be safe. Priya is on birth control pills for pregnancy prevention, but they are both unsure about STI protection. Rohan mentions he's not a big fan of condoms. They discuss their options, and their doctor advises them that while Priya's pills are great for preventing pregnancy, condoms are still essential for protecting against STIs, especially as they get to know each other better and are not yet sure about their STI status.
Have an open conversation with your partner(s) about your sexual health needs and preferences. If you're considering non-condom methods for pregnancy prevention, consult with a healthcare provider or a sexual health clinic. They can help you understand the effectiveness, risks, and benefits of each method, including diaphragms, sponges, hormonal contraceptives, and internal condoms. Remember, for penile sex, condoms offer unique protection against STIs that other methods do not. If STI prevention is a concern, condoms should be a part of your sexual health toolkit.
A1: For penile sex, condoms are the only method that offers significant protection against STIs. While some internal barrier methods might offer a slight reduction in risk for certain STIs, they are not as effective as condoms. Oral sex carries its own risks, and while dental dams can offer some protection during oral-vaginal or oral-anal sex, they are not foolproof. Open communication and regular STI testing are key.
A2: If you have a latex allergy, you can opt for non-latex external condoms made from materials like polyurethane or polyisoprene. For internal barrier methods, the internal condom (FC2) is latex-free. Diaphragms are typically made of silicone, which is also a good option for those with latex sensitivities.
A3: Hormonal methods like birth control pills, patches, and rings are highly effective, with typical use effectiveness rates often above 90% for pregnancy prevention. However, they do not protect against STIs.
A4: The pull-out method is considered a high-risk method for both pregnancy and STI prevention due to its low effectiveness and lack of barrier protection. It is generally not recommended as a primary method of contraception.
Nutrition labels are designed to inform — but food manufacturers often make them difficult to interpret. This expert guide walks through every section of a nutrition label, exposing the common tricks used to mislead consumers and showing you what to actually look for.
April 14, 2026
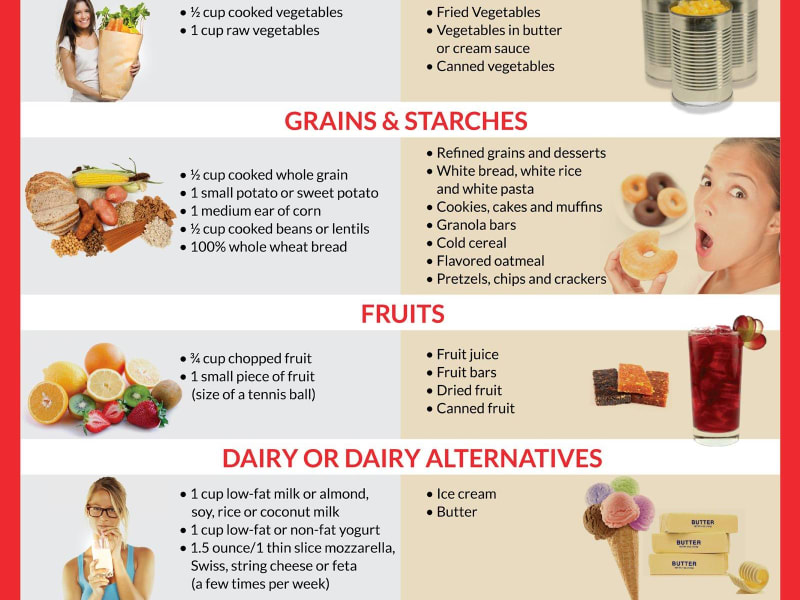
The carbohydrate debate is more nuanced than "eat less carbs." The quality of carbohydrates — their fibre content, processing level, and glycaemic impact — matters far more than their mere presence in your diet. Here's the science behind the distinction.
April 14, 2026

Most official protein recommendations were set to prevent deficiency — not to optimise health, muscle mass, or longevity. New research suggests the real requirements are significantly higher than the standard RDA, particularly for active adults and older populations.
April 13, 2026