Free Helpline
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
We are here to assist you.
Health Advisor
+91-8877772277Available 7 days a week
10:00 AM – 6:00 PM to support you with urgent concerns and guide you toward the right care.
Explore the realities of bareback sex, understanding its appeal, the significant health risks like STIs and unintended pregnancy, and crucial steps towards safer practices.

The term “bareback sex” might conjure up different images, but at its core, it means having penetrative sexual intercourse without using a barrier method, most commonly a condom. The phrase itself is a nod to horseback riding without a saddle. While the idea of direct skin-to-skin contact can be appealing to some, it’s essential to approach this topic with a clear understanding of the potential consequences. This isn't a decision to be made lightly, as the risks, especially concerning sexually transmitted infections (STIs) and unintended pregnancies, are significant.
Bareback sex refers to any form of penetrative sex where a condom or other barrier method is not used. This can include vaginal, anal, or oral sex, though the term is most commonly associated with penetrative acts. The origins of the term are linked to the gay press in the mid-1990s, initially referring to intentional condom-less anal sex among gay men living with HIV. Over time, its meaning broadened to encompass any penetrative sexual activity without a barrier.
Despite the considerable risks, some individuals are drawn to bareback sex for several reasons:
The risks associated with bareback sex are substantial and cannot be overstated. The absence of a barrier significantly increases the likelihood of transmitting and contracting various health issues.
According to the World Health Organization (WHO), over 1 million STIs are acquired every hour globally. Without a condom, the risk of transmission for a wide range of STIs is considerably higher. These include:
It's critical to understand that many STIs have no visible symptoms or symptoms so mild they go unnoticed. This is particularly true for HIV, which can be undetectable in its early stages. You or your partner could be unknowingly carrying and transmitting an infection. A common scenario is a couple who have been together for a while, decide to try bareback sex, and one partner unknowingly passes an STI to the other, leading to a difficult conversation and potential health consequences.
If pregnancy is not desired, bareback sex significantly increases the risk. While condoms are not 100% effective, they offer a substantial layer of protection against pregnancy. Without this barrier, sperm can more easily reach the egg, leading to an unintended pregnancy.
If you and your partner are considering bareback sex, it's imperative to have an open and honest conversation about the risks involved and your mutual expectations. Here are some steps to take:
Talk about your sexual history, STI status, and any concerns you both have. Discuss your desires, boundaries, and what you hope to gain from this experience. Honesty is the foundation of any safe sexual encounter.
Both partners should undergo comprehensive STI testing before engaging in bareback sex, and ideally, continue regular testing thereafter, especially if you have multiple partners. Knowing your status is the first step in protecting yourselves and others.
For individuals at higher risk of HIV exposure, PrEP is a highly effective medication that can significantly reduce the risk of contracting HIV. When taken as prescribed, PrEP can reduce the risk of HIV infection by about 99 percent. Discuss PrEP with your doctor to see if it's a suitable option for you.
If pregnancy is a concern, ensure that reliable birth control methods are in place. This could include hormonal contraceptives, IUDs, or other forms of contraception, used in conjunction with barrier methods if STIs are also a concern.
If possible, have open discussions about your partner's sexual health and testing history. However, remember that a partner's word is not a substitute for actual testing.
While not a substitute for condoms, using a good quality lubricant can reduce friction and potential tearing of tissues, which can decrease the risk of STI transmission. Opt for water-based or silicone-based lubricants, as oil-based lubricants can weaken latex condoms if they are used at any point.
It is advisable to consult a healthcare professional if:
Your doctor can provide personalized advice, conduct necessary tests, and discuss the most effective ways to protect your sexual health. Remember, making informed choices and prioritizing your well-being is paramount.
No, bareback sex does not prevent STIs. In fact, it significantly increases the risk of transmission and acquisition of STIs compared to sex with a condom.
While the absence of a barrier allows sperm to reach the egg directly, which might be seen as beneficial for conception, it comes with a much higher risk of STIs, some of which can negatively impact fertility and pregnancy outcomes. If conception is the goal, it's still wise to be tested for STIs.
Yes, HIV can be transmitted during bareback sex. The risk is higher, especially during anal sex. PrEP is a highly effective tool for preventing HIV transmission.
Signs can vary widely and often include unusual discharge, sores, warts, itching, burning during urination, or pain during sex. However, many STIs have no symptoms at all, making regular testing essential.
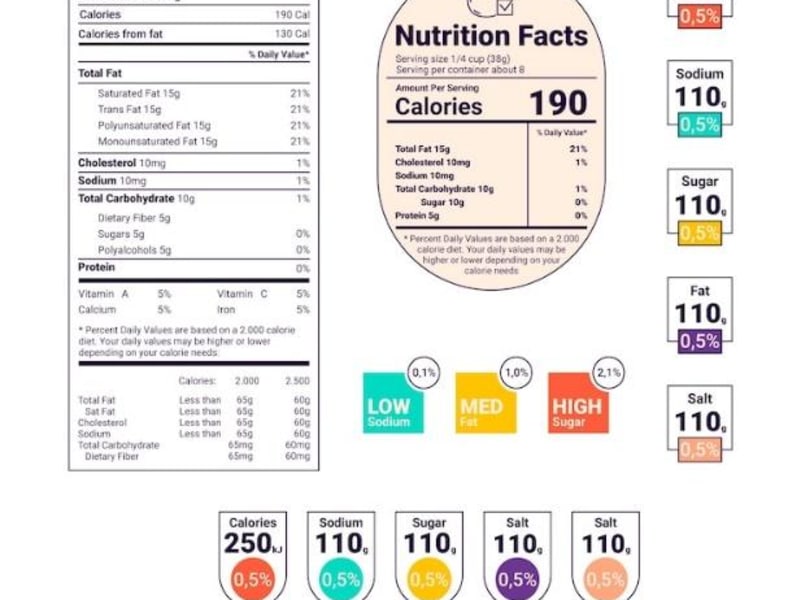
Nutrition labels are designed to inform — but food manufacturers often make them difficult to interpret. This expert guide walks through every section of a nutrition label, exposing the common tricks used to mislead consumers and showing you what to actually look for.
April 14, 2026
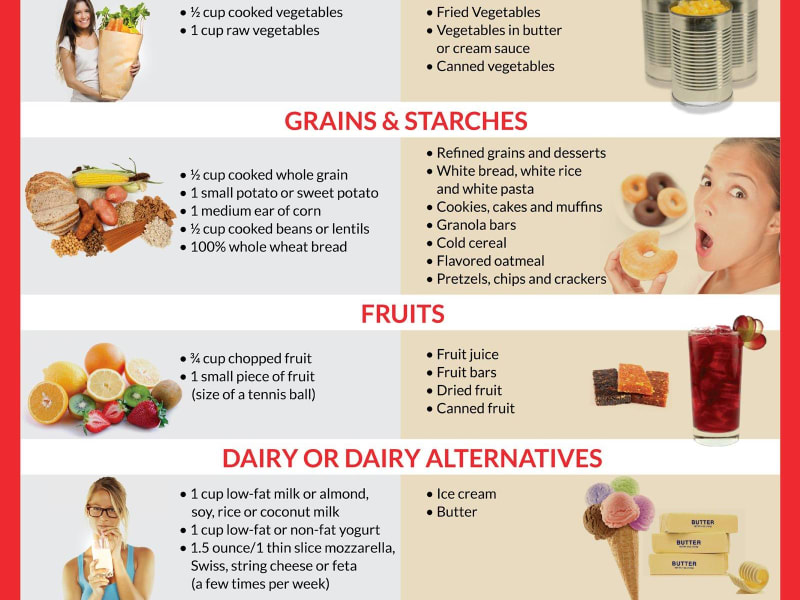
The carbohydrate debate is more nuanced than "eat less carbs." The quality of carbohydrates — their fibre content, processing level, and glycaemic impact — matters far more than their mere presence in your diet. Here's the science behind the distinction.
April 14, 2026

Most official protein recommendations were set to prevent deficiency — not to optimise health, muscle mass, or longevity. New research suggests the real requirements are significantly higher than the standard RDA, particularly for active adults and older populations.
April 13, 2026